Picture this: you feel unusually thirsty, run to the bathroom every hour, and drag through your day with unexplained fatigue. Most people brush these signs off. But they could be your body sending a very serious signal, one that 537 million adults worldwide are already living with.
That signal is diabetes.
Diabetes is not simply a “sugar problem.” It is a complex metabolic disorder that affects how your entire body processes energy. Left unmanaged, it silently damages your heart, kidneys, nerves, and eyes over the years. But here is the genuinely encouraging part: when caught early and managed consistently, most people with diabetes live full, active lives.
Whether you are newly diagnosed, a concerned family member, or simply someone who wants to understand a condition affecting 1 in 10 people globally, this guide is for you. No medical background required. Just clear, honest answers.

What is Diabetes? (Core Definition)
Diabetes is a chronic metabolic disorder in which the body cannot properly regulate blood glucose (blood sugar) either because it does not produce enough insulin or because its cells no longer respond to insulin correctly. The result is persistently high blood sugar that, over time, damages organs throughout the body.
In simpler terms: your body runs on glucose (sugar). Insulin, a hormone produced by your pancreas, acts like a key that unlocks your cells so glucose can enter and fuel them. In diabetes, this system breaks down. Glucose builds up in the bloodstream instead of reaching the cells, and the consequences compound over the years.
How the Body Normally Controls Blood Sugar
Under healthy conditions, your body maintains a careful blood sugar balance through a seamless process:
- You eat carbohydrates, which break down into glucose and enter your bloodstream.
- Your pancreas detects rising blood glucose and releases insulin from its beta cells.
- Insulin signals cells in your muscles, liver, and fat tissue to absorb that glucose.
- Blood sugar drops back to the normal range (70–99 mg/dL fasting).
- If blood sugar falls too low, the pancreas releases a second hormone, glucagon, to signal the liver to release stored glucose back into the blood.
This system runs automatically, dozens of times per day, without any conscious effort. Most people never think about it until it stops working.
What Goes Wrong in Diabetes
This elegant regulatory system fails in one of two key ways:
Insulin deficiency: The pancreas produces little or no insulin (the mechanism underlying Type 1 diabetes). Without insulin, glucose simply cannot enter the cells, no matter how much is present in the blood.
Insulin resistance: The body produces insulin, but cells gradually stop responding to its signals (a mechanism underlying Type 2 diabetes). The pancreas compensates by pumping out more and more insulin until it eventually can no longer keep up with demand.
Either way, the outcome is chronic high blood sugar, medically called hyperglycemia, which slowly corrodes blood vessels and nerves throughout the body.
Types of Diabetes Explained Simply
Diabetes is not a single disease. It is a family of related blood sugar disorders with different causes, mechanisms, and management strategies. Here are the four types everyone should understand.
Type 1 Diabetes
Type 1 diabetes is an autoimmune condition. The body’s immune system mistakenly identifies the insulin-producing beta cells of the pancreas as foreign invaders and destroys them. As a result, the pancreas produces no insulin whatsoever. Without insulin, survival is impossible; daily insulin replacement is required.
Type 1 most commonly develops in children, teenagers, and young adults, though it can appear at any age. It accounts for roughly 5–10% of all diabetes cases. It is not caused by diet or lifestyle and cannot be prevented with current knowledge. Managing Type 1 requires daily insulin injections or an insulin pump, blood sugar monitoring, and careful carbohydrate awareness.
Type 2 Diabetes
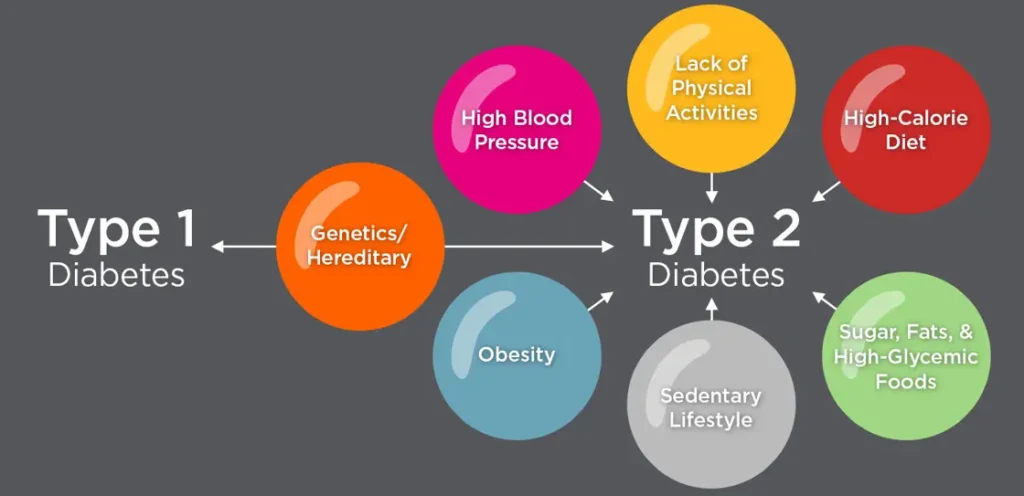
Type 2 diabetes is by far the most common form, accounting for over 90% of all diabetes diagnoses worldwide. It develops gradually as cells throughout the body become increasingly resistant to insulin’s signals. The pancreas produces more insulin to compensate, but over the years, it loses the capacity to keep up.
Type 2 is strongly linked to obesity, physical inactivity, poor dietary habits, and genetics. It is considered largely preventable and, in its earlier stages, often reversible through significant lifestyle changes. Many people, however, require oral medication or eventually insulin as the condition progresses.
Gestational Diabetes
Gestational diabetes develops during pregnancy in women who did not previously have diabetes. Hormones produced by the placenta block the normal action of insulin, leading to elevated blood sugar that can harm both mother and baby. It typically resolves after delivery, but it leaves a lasting imprint. Women who had gestational diabetes carry a 50–70% lifetime risk of developing Type 2 diabetes later in life. Their children also have a higher lifelong risk.
Prediabetes
Prediabetes is the critical early warning stage. Blood sugar is higher than normal but has not yet crossed the threshold for a diabetes diagnosis. This stage is fully reversible with lifestyle changes, yet 80% of the estimated 541 million people worldwide with prediabetes have no idea they have it. Prediabetes rarely causes obvious symptoms, which makes routine screening essential for anyone with risk factors.
Early Signs and Symptoms of Diabetes
The most common early warning signs of diabetes include frequent urination, excessive thirst, unexplained weight loss, persistent fatigue, blurred vision, slow-healing wounds, frequent infections, and tingling or numbness in the hands or feet.
Many people, particularly those with Type 2 diabetes or prediabetes, have no noticeable symptoms for years. This is why diabetes is often called a silent disease. When symptoms do appear, here is what to watch for:
- Frequent urination (polyuria): Excess glucose in the blood is filtered by the kidneys. When levels are too high, the kidneys flush it out in urine, taking a large amount of water with it.
- Excessive thirst (polydipsia): Fluid loss from frequent urination triggers intense thirst. This is often the first symptom people notice.
- Unexplained weight loss: Without insulin to allow glucose into cells, the body breaks down fat and muscle for energy, leading to rapid weight loss, especially pronounced in Type 1 diabetes.
- Persistent fatigue: Cells starved of glucose cannot produce energy efficiently, leaving a person exhausted regardless of how much sleep they get.
- Blurred or fluctuating vision: High blood sugar causes the lenses of the eyes to swell, temporarily distorting vision.
- Slow-healing wounds: High glucose impairs circulation and immune function, dramatically slowing the body’s ability to repair tissue damage.
- Frequent infections: Elevated blood sugar levels create an environment where bacteria and fungi thrive, leading to recurrent skin, gum, and urinary tract infections.
- Tingling or numbness in hands and feet: A sign that elevated glucose has already begun to affect nerve function, and is an early indicator of diabetic neuropathy.
- Fruity-smelling breath: A warning sign specific to Type 1 diabetes, indicating the body is burning fat for fuel and producing ketones, a potentially dangerous state called diabetic ketoacidosis (DKA).

Symptoms in Men vs Women
While most symptoms are shared, diabetes presents some gender-specific differences. Men may experience reduced libido, erectile dysfunction, and decreased muscle mass and strength. Women with undiagnosed diabetes are more susceptible to frequent yeast infections, urinary tract infections, and polycystic ovary syndrome (PCOS), a hormonal condition that is itself strongly tied to insulin resistance.
Symptoms in Children
Type 1 diabetes in children can progress rapidly over days or weeks. Parents should watch for sudden bedwetting in a previously toilet-trained child, dramatic weight loss despite a healthy appetite, extreme thirst, and unusual irritability or mood changes. In severe cases, a child may present in diabetic ketoacidosis, a life-threatening emergency requiring immediate hospital care. If you notice these signs in a child, seek urgent medical attention.
Causes and Risk Factors of Diabetes
Diabetes does not have a single cause. It results from a combination of genetic predisposition, environmental triggers, and, especially in Type 2, lifestyle choices accumulated over the years.
The key contributing factors include:
- Genetics and family history: Having a parent or sibling with diabetes meaningfully raises your risk. Certain gene variants increase susceptibility to both Type 1 and Type 2 diabetes, though genes alone are rarely the whole story.
- Obesity and excess body fat: Excess fat, particularly visceral fat stored around abdominal organs, triggers chronic, low-grade inflammation and directly interferes with insulin signaling, driving insulin resistance.
- Poor dietary habits: Diets high in ultra-processed foods, refined carbohydrates, and sugary beverages chronically spike blood sugar and insulin demand, gradually wearing down the pancreas’s capacity to respond.
- Lack of physical activity: Muscles are the body’s primary glucose consumers during movement. A sedentary lifestyle dramatically reduces the body’s ability to clear glucose from the blood.
- Hormonal imbalances: Conditions like polycystic ovary syndrome (PCOS), Cushing’s syndrome, and an overactive thyroid can impair insulin sensitivity and raise diabetes risk.
- Autoimmune dysfunction (Type 1): The immune system’s attack on beta cells is likely triggered by a combination of genetic vulnerability and environmental factors, possibly including certain viral infections.
- Age: The risk of Type 2 diabetes increases significantly after age 45, as insulin sensitivity naturally declines with aging.
Who is at Higher Risk?
You face a significantly elevated risk of developing Type 2 diabetes if you are over age 45, have a BMI above 25, carry excess abdominal weight, have a close family member with diabetes, are physically inactive, had gestational diabetes during a pregnancy, belong to a South Asian, African American, or Hispanic ethnic group, or have been diagnosed with prediabetes, high blood pressure, or abnormal cholesterol levels. The more risk factors that apply to you, the more urgently you need regular screening.
How Diabetes is Diagnosed
Diagnosing diabetes requires a simple blood test, no complex procedures, and no hospital stay. Here are the three gold-standard diagnostic tests used by doctors worldwide, along with what the numbers mean:
Fasting Blood Sugar (FBS): Taken after at least 8 hours without food. Normal is below 100 mg/dL. Prediabetes is 100–125 mg/dL. Diabetes is 126 mg/dL or higher on two separate occasions.
HbA1c (Glycated Hemoglobin): Measures your average blood sugar over the past 2–3 months by calculating what percentage of hemoglobin has glucose attached. Normal is below 5.7%. Prediabetes is 5.7%–6.4%. Diabetes is 6.5% or higher.
Oral Glucose Tolerance Test (OGTT): You drink a standardized glucose solution, and your blood sugar is measured two hours later. Normal is below 140 mg/dL. Prediabetes is 140–199 mg/dL. Diabetes is 200 mg/dL or higher.
Random Blood Sugar: A reading of 200 mg/dL or higher taken at any time, combined with classic diabetes symptoms, is sufficient to confirm a diagnosis.
What Do Test Results Mean?
The HbA1c test is especially valuable for diagnosis and ongoing management because it reflects weeks of blood sugar behavior rather than a single moment in time. It works by measuring how much glucose has bonded permanently to hemoglobin in red blood cells. Since red blood cells live roughly 90 days, the test gives a reliable three-month average. A result of 6.5% or higher on two separate tests confirms diabetes, while anything below 5.7% is considered normal.
If you are over 35, overweight, or have any risk factors, ask your doctor for a routine HbA1c test at your next visit — even if you feel perfectly well. Early detection before symptoms appear is your most powerful opportunity to prevent complications.
Why Diabetes is a Lifestyle Disease
Type 2 diabetes, by far the most common form globally, is fundamentally a disease of how modern people live. Genes load the gun, but lifestyle pulls the trigger. The extraordinary rise of Type 2 diabetes over the past four decades maps almost exactly onto the global rise of ultra-processed food consumption, desk-based sedentary work, chronic stress, disrupted sleep, and urban environments designed against physical movement.
The key lifestyle drivers are well established. Diets high in refined carbohydrates and added sugars cause dramatic, repeated spikes in blood glucose, triggering massive insulin responses. Over the years, cells progressively desensitize to insulin’s signals in response to this constant stimulation. Ultra-processed foods are engineered to promote overconsumption, leading to weight gain and chronic systemic inflammation, both of which directly impair insulin sensitivity. Sugary drinks deliver glucose directly into the bloodstream without fiber to slow absorption, making them particularly damaging. Chronic stress elevates cortisol, which raises blood sugar and encourages visceral fat accumulation. Even poor sleep, now well documented in research, significantly impairs insulin sensitivity after just a few consecutive nights.

Connection Between Obesity and Diabetes
The link between obesity and Type 2 diabetes is so well established that researchers coined the term “diabesity” to describe the parallel epidemic. Visceral fat, the fat stored around and inside abdominal organs, releases inflammatory chemicals called cytokines that directly disrupt insulin signaling pathways. The relationship is dose-dependent: the more visceral fat, the greater the insulin resistance.
The encouraging flip side is equally well documented. Losing just 5–10% of body weight produces measurable improvements in blood sugar control. Losing 15% or more has been shown in clinical trials, including the DiRECT trial published in The Lancet, to achieve complete remission of Type 2 diabetes in over half of participants. Biology is not fixed; it responds powerfully to how you live.
Complications if Diabetes is Not Controlled
Persistently elevated blood sugar is chemically corrosive to the body’s tissues. Excess glucose damages blood vessel walls and peripheral nerves through several mechanisms: glycation, oxidative stress, and chronic inflammation, leading to a cascade of serious complications that develop silently over the years.
Cardiovascular disease: Damaged and stiffened blood vessels accelerate atherosclerosis (the buildup of arterial plaques). People with diabetes are two to four times more likely to develop coronary heart disease or suffer a stroke compared to those without diabetes. Cardiovascular disease is the leading cause of death in people with diabetes.
Kidney damage (diabetic nephropathy): High blood glucose levels damage the kidneys’ tiny filtering units (glomeruli), progressively reducing their ability to filter waste. Diabetes is the leading cause of kidney failure worldwide, responsible for roughly 40% of all cases requiring dialysis.
Nerve damage (diabetic neuropathy): Affects over half of all people with long-standing diabetes. It most commonly causes tingling, burning pain, and numbness in the feet and legs. Because sensation is reduced, injuries go unnoticed, and infections can progress unchecked, sometimes requiring amputation.
Eye damage (diabetic retinopathy): High blood sugar weakens the tiny blood vessels of the retina, causing them to leak, swell, or grow abnormally. Diabetic retinopathy is the leading cause of blindness among working-age adults in high-income countries. Annual eye examinations are essential for catching it early.
Diabetic foot complications: The combination of impaired circulation and nerve damage turns what would be a minor foot blister or cut into a potentially limb-threatening infection. Regular foot inspection and proper footwear are non-negotiable for people with diabetes.
Cognitive decline: Growing research links poorly controlled Type 2 diabetes to a significantly increased risk of Alzheimer’s disease and vascular dementia, a connection so strong that some researchers have proposed calling Alzheimer’s “Type 3 diabetes,” though this remains under debate.
Why Early Detection Matters
Every single one of these complications is either preventable or significantly delayed with consistent blood sugar management. The landmark UKPDS (UK Prospective Diabetes Study) demonstrated that intensive blood sugar control in early Type 2 diabetes reduced the risk of microvascular complications by 25% over a 10-year period. The earlier management begins, the greater the protective benefit. Every year of good control matters.
Can Diabetes Be Controlled or Prevented?
Type 1 diabetes cannot currently be prevented. However, Type 2 diabetes is largely preventable and often reversible in its early stages through structured lifestyle changes, particularly a healthy diet, regular physical activity, weight management, and stress reduction.
The evidence here is unusually strong. The Diabetes Prevention Program (DPP), a major clinical trial funded by the US National Institutes of Health, demonstrated that participants who lost 5–7% of body weight through dietary changes and engaged in 150 minutes of moderate exercise per week reduced their risk of progressing from prediabetes to Type 2 diabetes by 58%. Among adults over 60, the risk reduction was 71%. These results outperformed the diabetes drug metformin, which reduced risk by 31% in the same study.
Practical prevention looks like this:
- Eat a balanced, lower-glycemic diet centered on vegetables, legumes, whole grains, lean proteins, and healthy fats, while minimizing refined carbohydrates and added sugars.
- Aim for at least 150 minutes of moderate aerobic exercise each week; brisk walking qualifies. Add two sessions of resistance training to significantly improve insulin sensitivity.
- Achieve and maintain a healthy weight. Even modest weight loss of 5–7% of body weight produces meaningful metabolic benefits.
- Prioritize 7–9 hours of quality sleep per night to support healthy cortisol and insulin rhythms.
- Manage chronic stress through whatever methods work for you, whether meditation, exercise, time in nature, or therapy.
- Stop smoking. Smokers are 30–40% more likely to develop Type 2 diabetes than non-smokers.
- Get regular blood sugar screenings, particularly if you have any risk factors. Finding prediabetes is your last and best opportunity to reverse course entirely.
Role of Prevention in Type 2 Diabetes
For those already diagnosed with Type 2 diabetes, the prevention goal shifts to preventing or delaying complications. This means working with your healthcare team to maintain HbA1c below 7%, managing blood pressure and cholesterol within target ranges, attending annual eye and foot examinations, and taking medications as prescribed. Many people achieve diabetes remission, defined as HbA1c below 6.5% for three or more months without glucose-lowering medication through substantial lifestyle changes, structured low-calorie dietary programs, or bariatric surgery. Remission is a realistic goal, not a fantasy, for a meaningful proportion of people with Type 2 diabetes.

Quick Summary | Key Takeaways
- Diabetes is a chronic metabolic disorder in which the body cannot properly regulate blood glucose due to insulin deficiency or insulin resistance.
- There are four main types: Type 1 (autoimmune), Type 2 (lifestyle-related and most common), Gestational (occurs during pregnancy), and Prediabetes (the fully reversible early warning stage).
- Common early symptoms include frequent urination, excessive thirst, fatigue, unexplained weight loss, and blurred vision, but many people have no symptoms at all for years.
- Type 2 diabetes is strongly driven by obesity, poor diet, physical inactivity, and genetics, all of which can be meaningfully addressed through lifestyle change.
- Diagnosis is confirmed via blood tests: Fasting Blood Sugar, HbA1c, or the Oral Glucose Tolerance Test.
- Uncontrolled diabetes causes serious, progressive complications, including heart disease, kidney failure, blindness, nerve damage, and cognitive decline.
- Type 2 diabetes is up to 58% preventable with diet and exercise intervention, even in high-risk individuals.
- Early detection and consistent management are the two most powerful tools available against diabetes progression.
Frequently Asked Questions
Is diabetes curable?
Type 1 diabetes currently has no cure, as the autoimmune damage to insulin-producing cells is permanent. Type 2 diabetes can go into remission, meaning blood sugar returns to normal levels without medication through significant weight loss and lifestyle change. However, this requires ongoing commitment to maintain; it is not a one-time fix. Prediabetes is fully and permanently reversible with the right lifestyle changes made early enough.
What causes diabetes in adults?
In adults, Type 2 diabetes is by far the most common form. It is caused by a combination of insulin resistance, where cells stop responding properly to insulin, and gradual pancreatic burnout. The key contributing factors are obesity (especially abdominal fat), physical inactivity, a diet high in refined carbohydrates and sugars, chronic stress, poor sleep, advancing age, and genetic predisposition. Certain ethnic groups, including South Asians, African Americans, and Hispanic individuals, also carry higher genetic susceptibility. It is worth noting that Type 1 diabetes can also develop in adults, a condition known as LADA (Latent Autoimmune Diabetes in Adults), and is frequently misdiagnosed as Type 2.
Can diet alone control diabetes?
For prediabetes, dietary changes alone can often normalize blood sugar levels completely. For early or mild Type 2 diabetes, a well-structured diet, particularly a low-carbohydrate or Mediterranean-style eating pattern, can dramatically reduce HbA1c, sometimes into the normal range. However, most established cases of Type 2 diabetes require a combination of diet, regular physical activity, and medication for optimal control. Type 1 diabetes always requires insulin therapy regardless of diet, though eating well significantly reduces the amount of insulin needed and improves overall control.
How do I know if I am prediabetic?
Prediabetes almost never causes noticeable symptoms, which is exactly why the vast majority of people with it go undiagnosed. The only reliable way to find out is through a blood test. A fasting blood sugar reading of 100–125 mg/dL, or an HbA1c of 5.7%–6.4%, confirms prediabetes. If you are over 35, overweight, physically inactive, or have a family history of diabetes, ask your doctor to include a blood sugar screening in your next routine checkup, even if you feel completely fine and have no symptoms.
What is the normal blood sugar level?
A normal fasting blood sugar level measured after at least 8 hours without food is below 100 mg/dL. Two hours after eating, a normal reading is below 140 mg/dL. A normal HbA1c is below 5.7%. A fasting reading of 100–125 mg/dL indicates prediabetes, and 126 mg/dL or higher on two separate occasions confirms diabetes. A random (non-fasting) reading of 200 mg/dL or higher, combined with diabetes symptoms, is also diagnostic. Your doctor interprets these numbers in the context of your full health picture.
This article was written following evidence-based guidelines from the American Diabetes Association (ADA) and the International Diabetes Federation (IDF). It is intended for educational purposes only. Always consult your physician or a qualified healthcare professional for personal medical advice, diagnosis, or treatment.














