Diabetes is one of the fastest-growing health crises of our time. Whether you’ve just been diagnosed, have a family member living with it, or simply want to understand the condition better, knowing the different types of diabetes is the first step toward better outcomes.
According to the IDF Diabetes Atlas 2025, 589 million adults worldwide are currently living with diabetes, which is 1 in 9 people. The condition caused 3.4 million deaths in 2024, one every 9 seconds, and cost the global healthcare system over $1 trillion. By 2050, that number is projected to reach 853 million people.
What Are the Different Types of Diabetes?
Diabetes is not a single disease. It’s a group of metabolic conditions that all share one thing in common: difficulty regulating blood sugar (glucose). The difference lies in why that regulation breaks down and that’s what separates one type from another.
Why Diabetes Is Not Just One Disease
Think of the different types of diabetes the way you’d think of different engine problems causing the same warning light on a car. The symptom of high blood sugar looks similar, but the cause is completely different. An autoimmune attack, insulin resistance, pregnancy hormones, or a genetic mutation each point to a different condition requiring a different treatment plan.
How Doctors Classify Diabetes Types
Doctors classify diabetes primarily by its root cause and mechanism. The main recognized types are Type 1, Type 2, gestational diabetes, and prediabetes. Rarer forms, including LADA, MODY, neonatal diabetes, and secondary diabetes, affect smaller populations but require equally specific management.
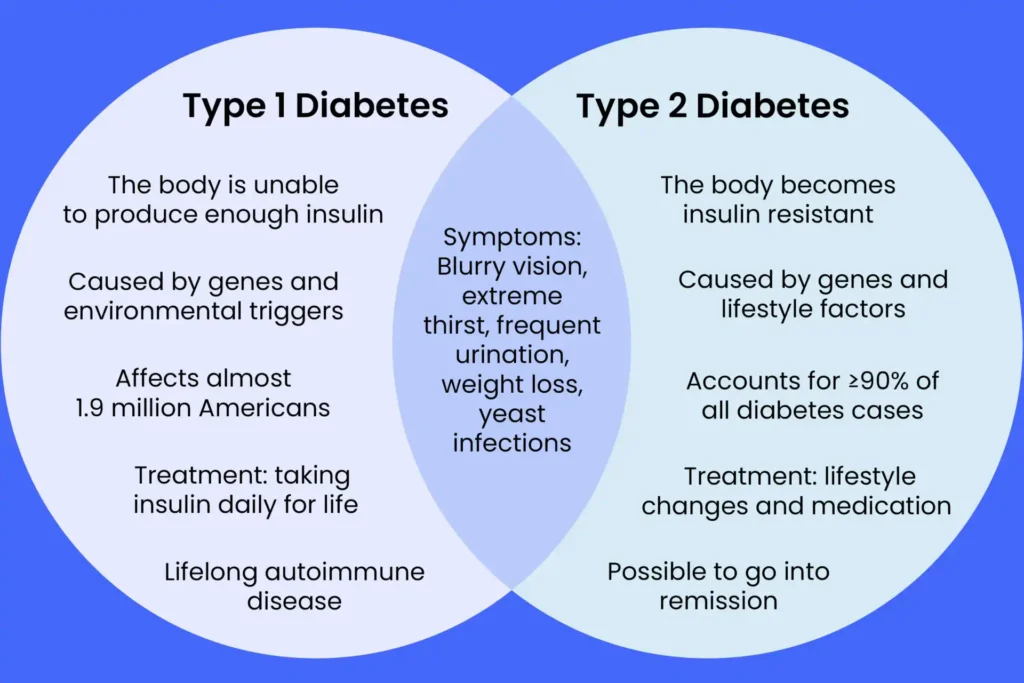
Type 1 Diabetes
What Is Type 1 Diabetes?
Type 1 diabetes is an autoimmune condition where the immune system mistakenly destroys the insulin-producing beta cells in the pancreas. The result is little to no insulin production, leaving glucose unable to enter cells for energy use. It accounts for 8–10% of all diabetes cases worldwide.
Formerly called juvenile diabetes, it most commonly appears in children, teenagers, and young adults, but it can develop at any age.
Causes of Type 1 Diabetes
The exact trigger remains unclear, but research points to a combination of genetic predisposition (specific HLA gene variants), environmental triggers such as viral infections, and an autoimmune response that turns the body’s defenses against its own tissue.
Symptoms of Type 1 Diabetes
Symptoms often appear suddenly and intensely:
- Extreme thirst and frequent urination
- Rapid, unexplained weight loss
- Severe fatigue and weakness
- Blurred vision
- Fruity-smelling breath (a warning sign of diabetic ketoacidosis, a medical emergency)
Who Is Most at Risk?
Children, teenagers, and young adults are most commonly diagnosed, especially those with a first-degree relative (parent or sibling) who has Type 1. Certain viral infections in early childhood may also trigger the autoimmune response in genetically susceptible individuals.
Treatment Options for Type 1 Diabetes
Type 1 diabetes cannot be prevented or reversed. Lifelong insulin therapy is essential. Treatment typically includes multiple daily insulin injections or a continuous insulin pump, regular blood glucose monitoring (including continuous glucose monitors, or CGMs), and a carbohydrate-aware diet paired with consistent physical activity.
Complications of Untreated Type 1 Diabetes
Without proper insulin management, Type 1 diabetes can lead to diabetic ketoacidosis (DKA), a life-threatening emergency. Long-term complications include cardiovascular disease, kidney failure, nerve damage, and vision loss.
Type 2 Diabetes
What Is Type 2 Diabetes?
Type 2 diabetes is by far the most common form, accounting for over 90% of all diabetes cases globally. Unlike Type 1, the pancreas still produces insulin, but the body’s cells become resistant to it, so glucose accumulates in the bloodstream rather than entering cells for fuel.
Causes of Type 2 Diabetes
Type 2 is driven by a combination of lifestyle and genetic factors: obesity and excess visceral (belly) fat, physical inactivity, a diet high in processed foods and refined sugars, family history of diabetes, and age over 45. Notably, rates are rising sharply in younger adults and even adolescents as childhood obesity increases worldwide.
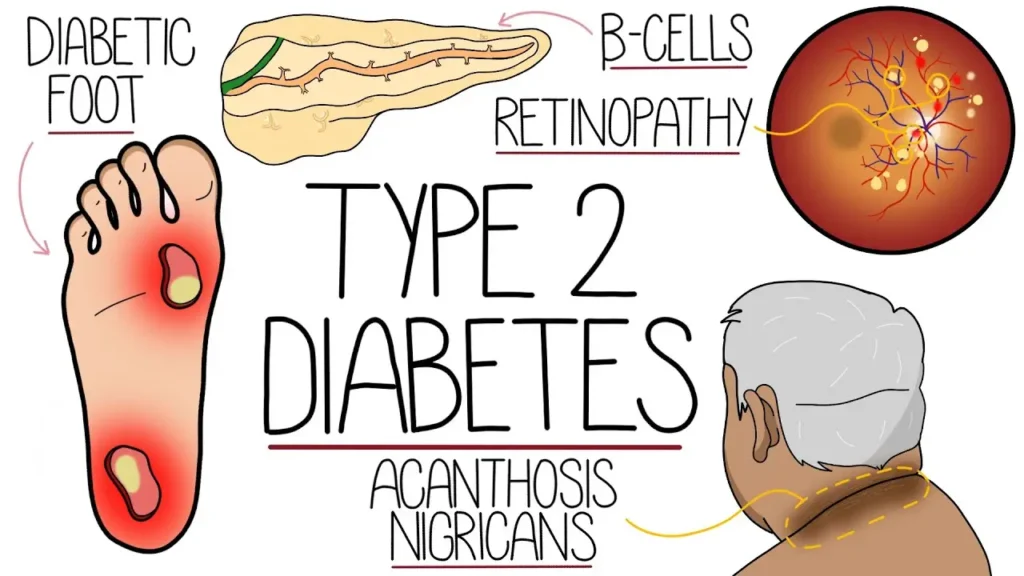
Early Symptoms of Type 2 Diabetes
Type 2 often develops slowly, with symptoms so subtle they go unnoticed for years:
- Blurred vision
- Tingling or numbness in the hands and feet
- Slow-healing wounds and frequent infections
- Dark, velvety skin patches around the neck or armpits (acanthosis nigricans)
- Increased hunger despite eating regularly
Can Type 2 Diabetes Be Reversed?
Yes, in many cases. Studies show that losing 5–10% of body weight through dietary changes and exercise can bring blood sugar levels back to normal, a state called diabetes remission. The NHS DiRECT trial found that 46% of participants achieved remission within one year through a structured low-calorie diet. This is one of the most important and underreported facts about Type 2 diabetes.
Best Treatment Options
Treatment follows a stepped approach: start with dietary changes and a low-glycaemic-index (GI) eating plan, add regular aerobic exercise (minimum 150 minutes per week), then introduce oral medications such as metformin. Newer drug classes, GLP-1 receptor agonists and SGLT2 inhibitors have shown impressive results in both blood sugar control and cardiovascular protection. Insulin is reserved for advanced cases.
Long-Term Risks of Type 2 Diabetes
People with Type 2 diabetes face a 2–4 times higher risk of cardiovascular disease. It is also the leading cause of kidney failure, preventable blindness, and non-traumatic lower-limb amputation globally.
Gestational Diabetes
What Is Gestational Diabetes?
Gestational diabetes develops during pregnancy, typically in the second or third trimester when pregnancy hormones interfere with insulin function, causing blood sugar to rise. It affects an estimated 1 in 6 pregnancies worldwide, according to the IDF Diabetes Atlas 2025.
Causes of Gestational Diabetes
Pregnancy naturally induces some degree of insulin resistance to ensure the baby receives enough glucose. In some women, the pancreas can’t compensate by producing extra insulin, and blood sugar rises above normal. Risk factors include pre-pregnancy overweight or obesity, family history of Type 2 diabetes, previous gestational diabetes, age over 25, and polycystic ovary syndrome (PCOS).
Symptoms of Gestational Diabetes
Gestational diabetes often has no noticeable symptoms, which is why routine screening between weeks 24–28 of pregnancy is standard practice in most countries.
Risks for Mother and Baby
If unmanaged, gestational diabetes raises the risk of the baby growing larger than normal (macrosomia), making delivery difficult. It also increases the risk of premature birth, respiratory issues for the newborn, and low blood sugar in the baby after birth. For the mother, it significantly raises the lifetime risk of developing Type 2 diabetes by up to 50% within 5–10 years.
How Gestational Diabetes Is Managed
Most cases are controlled through a carefully structured meal plan, regular blood sugar monitoring, and moderate physical activity. Some women require insulin or oral medication during pregnancy.
Does Gestational Diabetes Go Away After Pregnancy?
Yes. It typically resolves within weeks of delivery. However, it is a strong warning sign for future metabolic health, and women who experience it are encouraged to retest annually and maintain healthy lifestyle habits over the long term.
Prediabetes
What Is Prediabetes?
Prediabetes is a borderline blood sugar stage higher than normal, but not yet high enough to be classified as Type 2 diabetes. The IDF estimates that 634.8 million adults worldwide had impaired glucose tolerance in 2024, with many completely unaware of it.
Warning Signs of Prediabetes
Prediabetes often presents no symptoms at all. When signs do appear, they may include persistent fatigue, increased hunger or thirst, and dark skin patches around the neck or armpits. A simple HbA1c blood test can detect it.
Main Causes of Prediabetes
The causes mirror those of Type 2 diabetes: obesity, a diet high in refined carbohydrates and sugars, physical inactivity, family history, and chronic stress.
Can Prediabetes Be Reversed Naturally?
Yes, and this is where intervention matters most. The CDC Diabetes Prevention Program found that lifestyle changes reduced the progression from prediabetes to Type 2 diabetes by 58% overall, and by 71% in adults over 60. The formula is straightforward: lose 5–7% of body weight, exercise at least 150 minutes per week, and reduce sugar and refined carbohydrate intake.
How to Prevent Prediabetes from Becoming Type 2 Diabetes
Regular HbA1c testing, weight management, a low-GI, fiber-rich diet, and consistent physical activity are the most evidence-based strategies. Some high-risk individuals may also benefit from metformin under physician guidance.
Rare Types of Diabetes
What Is LADA Diabetes?
LADA (Latent Autoimmune Diabetes in Adults) is sometimes called Type 1.5 diabetes. It shares the autoimmune mechanism of Type 1 but progresses much more slowly, often being initially misdiagnosed as Type 2 because it appears in adults. People with LADA eventually require insulin, though this may take years.
What Is MODY Diabetes?
MODY (Maturity-Onset Diabetes of the Young) is a rare genetic form caused by a mutation in a single gene affecting insulin production. It accounts for roughly 1–2% of all diabetes diagnoses and is passed directly from parent to child with a 50% probability. Importantly, many MODY subtypes respond to oral sulfonylurea medication rather than insulin, making the correct diagnosis financially and medically significant.
Secondary Diabetes Explained
Secondary diabetes is caused by another condition or treatment, most commonly prolonged corticosteroid use, pancreatitis, Cushing’s syndrome, or certain surgeries. Managing the underlying cause often improves blood sugar control.
Neonatal Diabetes
One of the rarest forms of diabetes, neonatal diabetes occurs in babies under six months old due to genetic mutations. It may be transient (resolving within months) or permanent (requiring lifelong treatment).
Type 1 vs Type 2 Diabetes
| Feature | Type 1 Diabetes | Type 2 Diabetes |
| Root Cause | Insulin resistance in the body’s cells | Insulin resistance in body’s cells |
| Insulin Production | Very little or none | Produced but not used effectively |
| Onset Speed | Sudden (weeks) | Gradual (often years) |
| Typical Age Group | Children, teens, young adults | Adults (rising in youth) |
| Lifestyle Preventable? | No | Often yes |
| Can It Be Reversed? | No | Remission possible |
| Primary Treatment | Lifelong insulin therapy | Diet, exercise, oral meds, insulin |
| Share of Global Cases | ~8–10% | Over 90% |
Which Type of Diabetes Is More Dangerous?
Both types carry serious risks when unmanaged. Type 1 carries a higher immediate risk of diabetic ketoacidosis, while Type 2 is more closely linked to cardiovascular disease due to its association with metabolic syndrome. In practice, complications from both types are largely preventable with consistent care.
Can Type 2 Diabetes Turn Into Type 1?
No. They are fundamentally different diseases. However, people with long-standing Type 2 may eventually need insulin if the pancreas progressively loses function. This is sometimes misinterpreted as “turning into Type 1,” but the underlying mechanism remains insulin resistance, not autoimmune destruction.
Common Symptoms Shared by All Types of Diabetes
While each type has its own profile, several symptoms overlap across all forms of diabetes, particularly when blood sugar is elevated:
- Excessive thirst (polydipsia)
- Frequent urination (polyuria)
- Fatigue and weakness
- Blurred vision
- Slow-healing wounds and recurring infections
These shared symptoms explain why many people don’t know which type they have or that they have diabetes at all, without a blood test.
How Doctors Diagnose Different Types of Diabetes
HbA1c Test
The most common diagnostic tool. It measures average blood sugar over 2–3 months. An HbA1c of 5.7–6.4% indicates prediabetes; 6.5% or above confirms diabetes.
Fasting Blood Sugar Test
Taken after 8 hours of fasting. A reading of 100–125 mg/dL indicates prediabetes; 126 mg/dL or above on two occasions confirms diabetes.
Oral Glucose Tolerance Test
The patient drinks a glucose solution, and blood sugar is measured 2 hours later. This is the standard test for diagnosing gestational diabetes.
Antibody Testing for Type 1 Diabetes
Detects immune markers such as anti-GAD and islet cell antibodies, which confirm autoimmune destruction of the pancreas. Crucial for correctly diagnosing Type 1 or LADA in adults who may initially appear to have Type 2.
Can Diabetes Be Prevented?
Type 1 diabetes cannot currently be prevented. Type 2 diabetes, gestational diabetes, and prediabetes all respond to prevention strategies:
- Maintaining a healthy body weight
- Eating a Mediterranean-style or low-GI diet
- Exercising regularly
- Limiting alcohol and avoiding smoking
- Managing stress and prioritizing sleep
These strategies don’t just lower diabetes risk; they also reduce the risk of cardiovascular disease, certain cancers, and metabolic syndrome.
Living With Diabetes
Daily blood sugar management, structured meal planning, stress control, and adequate sleep all play medically validated roles in outcomes for people with diabetes. Stress raises cortisol, which in turn raises blood sugar, making emotional well-being a clinical priority rather than just a lifestyle preference. Research also shows that poor sleep worsens insulin resistance, even in healthy individuals.
The key takeaway for anyone living with any type of diabetes: consistency in small habits beats perfection in occasional ones.
Complications Linked to Different Diabetes Types
Over the long term, unmanaged high blood sugar damages blood vessels and nerves throughout the body. Key complications include cardiovascular disease (the leading cause of death among people with diabetes), kidney damage (the leading cause of kidney failure worldwide), nerve damage affecting up to 50% of long-term patients, retinopathy leading to preventable blindness, and diabetic foot problems that in severe cases require amputation.
The critical point: most of these complications are preventable with well-managed blood sugar, blood pressure, and cholesterol.
Key Takeaways
- Diabetes is not one disease; each type has distinct causes, mechanisms, and treatments
- Type 1 is autoimmune and requires lifelong insulin; Type 2 is driven by insulin resistance and is often preventable
- Gestational diabetes usually resolves after birth, but signals significant future risk
- Prediabetes is reversible; early action is the highest-leverage intervention
- Nearly half of all people with diabetes are undiagnosed; routine testing saves lives
- All types share common complications that are largely preventable with consistent management
Frequently Asked Questions
What are the main types of diabetes?
The main types are Type 1, Type 2, gestational diabetes, and prediabetes. Rarer forms include LADA (Latent Autoimmune Diabetes in Adults), MODY (Maturity-Onset Diabetes of the Young), neonatal diabetes, and secondary diabetes caused by other conditions or medications.
Which type of diabetes is hereditary?
MODY is the most directly hereditary, caused by a single-gene mutation, with a 50% chance of being passed to children. Type 2 also has a strong family history component. Type 1 carries genetic risk factors but is not directly inherited.
Can children get Type 2 diabetes?
Yes. While once rare in childhood, rising obesity rates have led to a significant global increase in Type 2 diagnoses among children and teenagers. The IDF notes that both Type 1 and Type 2 prevalence are rising in people under 20.
Is gestational diabetes permanent?
No. It typically resolves within weeks of delivery. However, women who develop it are up to 50% more likely to develop Type 2 diabetes within 5–10 years, making long-term lifestyle monitoring essential.
Can prediabetes go away?
Yes. With sustained lifestyle changes, such as losing 5–7% of body weight, following a low-sugar diet, and exercising consistently, prediabetes can be fully reversed and blood sugar returned to the normal range.
What is the rarest form of diabetes?
Neonatal diabetes, appearing in babies under six months old, is among the rarest. MODY accounts for only 1–2% of all global diabetes diagnoses. Both require specialist diagnosis as they are frequently misclassified.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional for diagnosis and treatment. Statistics sourced from the IDF Diabetes Atlas 11th Edition (2025) and peer-reviewed publications.













